Help! My Dental Assistant Won’t Learn New Things!
Don’t be the dental assistant who won’t learn new things.Find comfort in the new thing – even if the new things are scary at first. By: Ronda Holman Hi dear reader, my name is Ronda Holman and I have been sitting across from a dentist for a living for the last 25 years. I thought…
Read MoreWhy Do I Keep Having to Adjust the Anterior Teeth When Restoring?
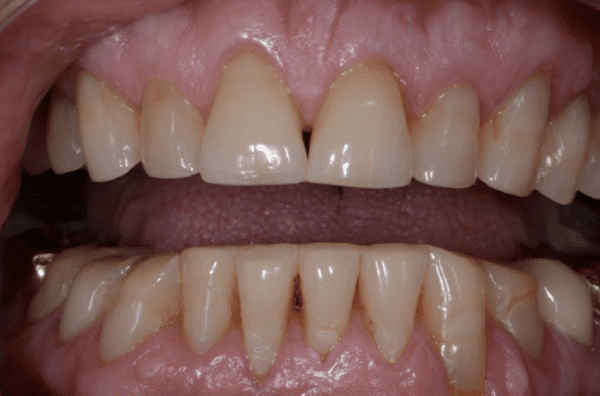
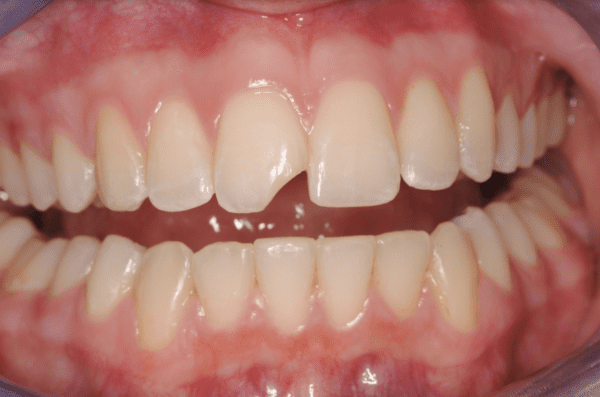
By: Dr. Leonard A. Hess, DDSClinical Director, The Dawson AcademyThe Article Originally Appeared on TheDawsonAcademy.com One of the main problems we see when we are restoring an anterior tooth that’s just recently chipped is that we always have to adjust occlusion. Whenever you see a chipped tooth you have to ask yourself why. Why is that chip there?…
Read MoreNew Year, New Approach? Shifting Your Financial Mentality
By: Todd Doobrow, CFP Your life as a doctor is complex in many ways. It started with dental school – additional years of training accompanied by hundreds of thousands of dollars in student loans. And as can be expected the focus of your classes was clinical; doctors get very little business training. Upon graduation, starting salaries…
Read MoreDr. William Chen Shares a Clinical Mistake and the Importance of Digital Dentistry
Host: Dr. Tanya Sue MaestasGuest: Dr. William ChenEdited By: Candy Velez CRDH We had the pleasure of speaking with Dr. Bill Chen, a highly successful dentist based in Sebring, Florida. Dr. Chen shares his insights and experiences, including a clinical mistake he made and how it relates to the world of digital dentistry. Building a…
Read MoreHow to Use Splints in Your Treatment Plan
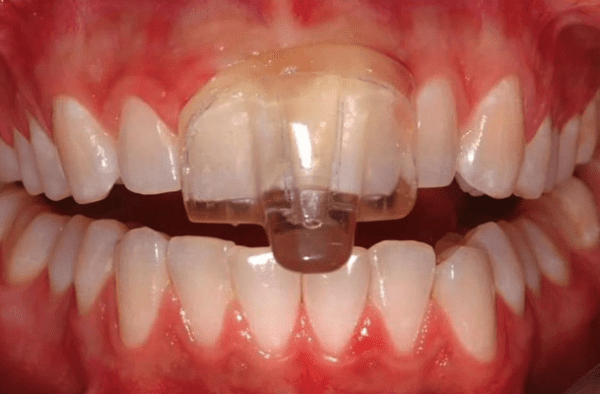
By: Dr. Leonard A. Hess, DDSClinical Director, The Dawson AcademyThe Article Originally Appeared on TheDawsonAcademy.com Hi, everybody, my name’s Dr. Leonard Hess. I’m one of the senior faculty members at the Dawson Academy. I’d like to spend a few minutes talking with you about where splints, or occlusal splints, work into a treatment plan when…
Read MoreNot Sure What To Do With Your Career in Dentistry? So, Now What?
By: Dr. Bri Torgerson I’m Dr. Bri Torgerson and I am a General Dentist working in Saint Louis, Missouri. I guess I’ll use the term “working” lightly. The truth is, I’ve been unemployed for the majority of this year, and not necessarily by choice. I went back and forth about writing this, about slicing my…
Read MoreImportance of Communication & Respect in Dental Teams: From the Perspective of a Dental Assistant
Interviewer: Tanya Sue Maestas, DDSInterviewee: Ronda HolmanEdited By: Candy Velez – CRDH, BSDH Today, we explore the vital role played by dental assistants, shedding light on the often-unnoticed significance of effective communication and respect within dental teams. Our guest, Ronda Holman, shares her experiences and insights, emphasizing the impact these factors can have on the…
Read MoreWhy am I Experiencing Clinical Failures?
By: Dr. Leonard A. Hess, DDSClinical Director, The Dawson AcademyThe Article Originally Appeared on TheDawsonAcademy.com If we’ve been practicing for any length of time at all, we’re going to see some clinical failures. I think sometimes the perception is if we’re faculty at The Dawson Academy, that it never happens, and you should know that…
Read MoreNavigating Professional Boundaries & Fair Compensation with Dental Assistant, Ronda Holman
In the intricate dance of professional boundaries & fair compensation,dental assistants often find themselves walking a tightrope. Interviewer: Tanya Sue Maestas, DDSInterviewee: Ronda HolmanEdited By: Candy Velez – CRDH, BSDH Today we explore the financial mistakes that dental assistants can make and the valuable lessons we can all learn from them. Ronda Holman shares her…
Read MoreWhat Script Do I Need To Order an MRI for a Patient?
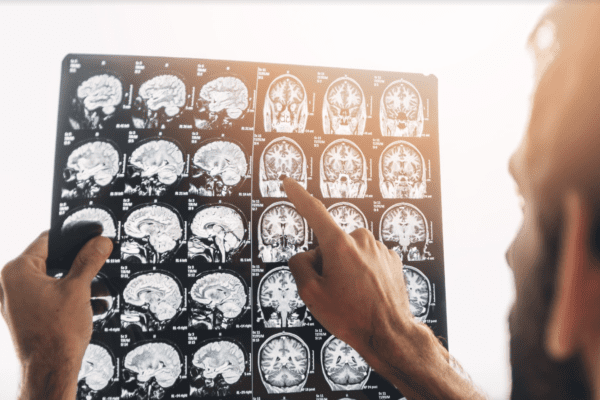
By: Dr. Leonard A. Hess, DDSClinical Director, The Dawson AcademyArticle Originally Appeared on TheDawsonAcademy.com So what script do we need if we order an MRI on our patient? Now, it used to be, several years ago, that MRI was kind of the gold standard for us to look inside the joint. That is not the…
Read More